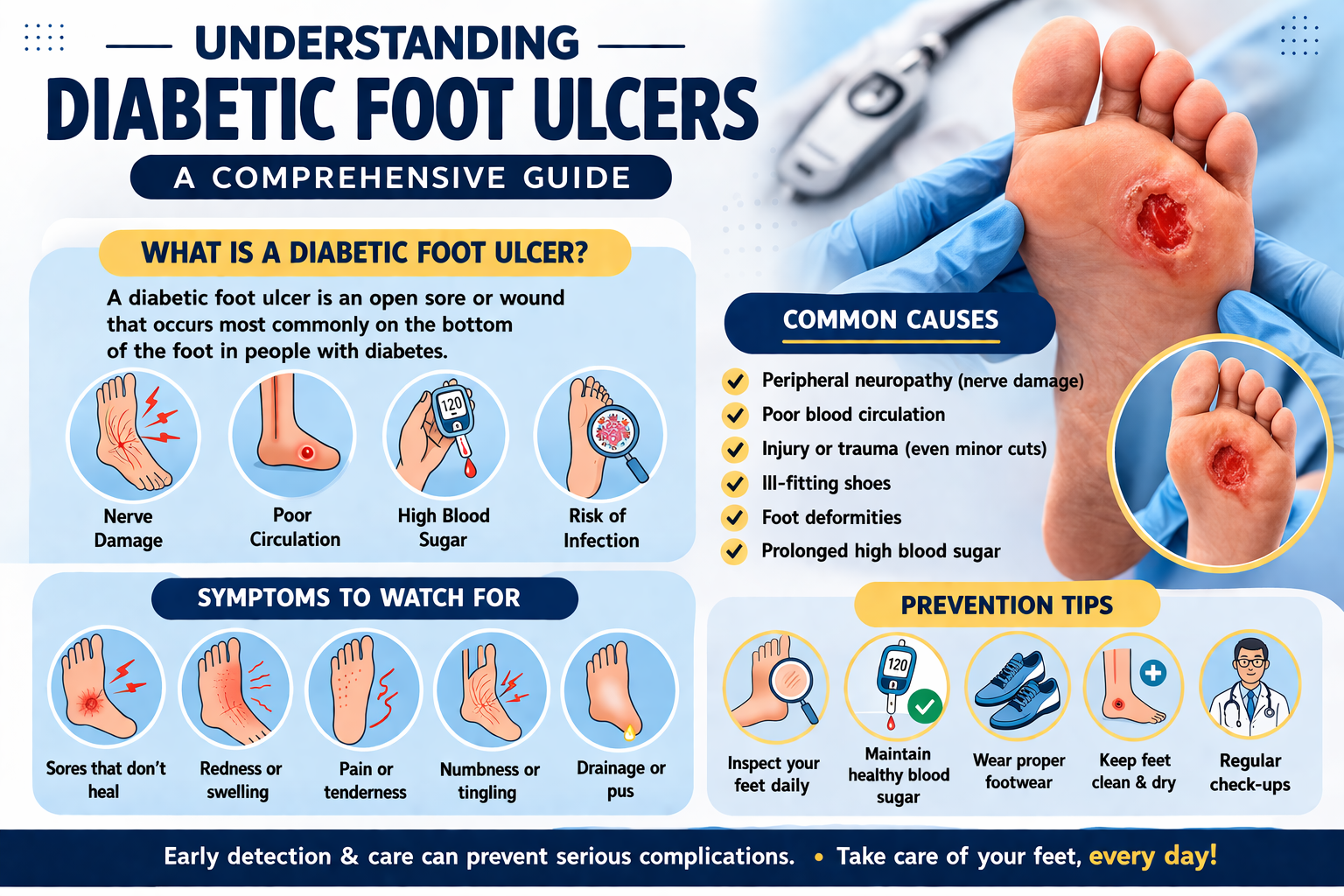
Why Foot Care Is a Non-Negotiable Priority for Diabetics
For the millions of people living with diabetes worldwide, foot care is not merely a cosmetic concern — it is a critical health imperative. Diabetes can cause a range of complications that make the feet extremely vulnerable to injury, infection, and in severe cases, amputation. According to the American Diabetes Association, people with diabetes are up to 30 times more likely to undergo a lower limb amputation than those without the condition. The sobering reality is that most of these amputations begin with a small, seemingly insignificant wound that was left untreated.
The good news? The vast majority of diabetes-related foot complications are entirely preventable. With a consistent, thorough daily foot care routine, you can dramatically reduce your risk of developing serious problems. Whether you were recently diagnosed or have been managing diabetes for years, establishing and sticking to a daily foot care regimen is one of the most powerful things you can do for your long-term health and quality of life.
In this comprehensive guide, we’ll walk you through exactly why diabetics need special foot care, what complications to watch out for, and most importantly, a complete step-by-step daily routine that you can begin implementing today.
Understanding Why Diabetes Affects Your Feet
Before diving into the routine itself, it’s important to understand the underlying reasons why diabetics must pay such careful attention to their feet. There are two primary diabetes-related conditions that put the feet at risk:
Diabetic Peripheral Neuropathy
High blood sugar levels over time can damage the nerves throughout your body, a condition known as diabetic neuropathy. When this damage occurs in the feet and legs, it’s called peripheral neuropathy. This condition can cause a range of sensations — tingling, burning, or numbness — and over time, may lead to a complete loss of feeling in the feet.
The danger here is profound: if you cannot feel pain, you may not notice cuts, blisters, ulcers, or foreign objects lodged in your foot. A small pebble in your shoe, for example, could rub a wound for hours without you realizing it. That wound, left unnoticed and untreated, can quickly become infected and deteriorate into a serious ulcer.
Peripheral Artery Disease (PAD)
Diabetes also increases the risk of peripheral artery disease, a condition in which the blood vessels in the legs and feet narrow, reducing blood flow to the extremities. Poor circulation means that even minor wounds heal much more slowly, and the immune system’s ability to fight infection in those areas is significantly compromised. When a wound doesn’t receive adequate blood supply, the tissue can begin to die, leading to a condition called gangrene.
Together, neuropathy and poor circulation create a dangerous combination that can turn a tiny cut into a life-altering medical emergency. This is precisely why a daily foot care routine isn’t optional — it’s essential.
The Complete Daily Foot Care Routine for Diabetics
The following routine is designed to be performed every single day. Think of it as a ritual — just like brushing your teeth or taking your medication. Consistency is the key to catching problems early and keeping your feet healthy for the long term.
Step 1: Wash Your Feet Every Day
Begin each day — or end it, whichever you prefer — by washing your feet thoroughly with warm (not hot) water and mild soap. This simple act removes bacteria, dirt, and sweat that can lead to infections.
- Use warm water, not hot: Because neuropathy may reduce your ability to sense temperature, it’s easy to unknowingly burn your feet with hot water. Always test the water temperature with your elbow or a thermometer. Aim for a temperature between 95°F and 100°F (35°C to 38°C).
- Avoid soaking your feet: Contrary to popular belief, soaking your feet for long periods can actually dry out the skin and increase the risk of cracking. A quick, thorough wash of 3–5 minutes is ideal.
- Wash between the toes: Fungal infections and moisture buildup love the spaces between the toes. Make sure you clean these areas carefully every day.
- Use a gentle, fragrance-free soap: Harsh or heavily fragranced soaps can strip the skin of its natural oils, leading to dryness and cracking.
Step 2: Dry Your Feet Thoroughly
Drying your feet is just as important as washing them. Moisture left on the skin — especially between the toes — creates a breeding ground for fungal infections like athlete’s foot, which can quickly become serious in diabetics.
- Pat, don’t rub: Gently pat your feet dry with a soft, clean towel rather than rubbing vigorously, which can cause skin irritation or damage fragile skin.
- Pay special attention to the spaces between your toes: Use a corner of the towel or a separate clean cloth to carefully dry between each toe.
- Consider a clean towel each time: Using the same towel repeatedly without washing it can reintroduce bacteria. If possible, use a fresh towel or wash your foot towels frequently.
Step 3: Inspect Your Feet Carefully
This step is arguably the most critical part of the entire routine. Daily foot inspections allow you to catch small problems before they become serious ones. Because neuropathy may prevent you from feeling wounds or irritation, your eyes become your most important diagnostic tool.
Set aside a few minutes each day to examine your feet in good lighting. Here’s what to look for:
- Cuts, scrapes, or wounds: Even the smallest break in the skin can become infected. Look carefully across the entire surface of each foot.
- Blisters: Blisters can form from friction or heat. Never pop a blister, as this opens the skin to infection. Cover it with a clean bandage and contact your doctor.
- Redness or swelling: Redness, warmth, or swelling can indicate an infection or the beginning of a pressure sore or ulcer.
- Calluses or corns: Hard, thickened areas of skin can develop into deeper wounds if not properly managed. Never cut them yourself with sharp instruments.
- Cracks or dry skin: Dry, cracked skin — especially around the heels — can deepen and become infected wounds.
- Changes in skin color: Unusual discoloration, such as dark patches, pale skin, or blue-tinged toes, can indicate poor circulation and should be evaluated by a doctor.
- Nail problems: Look for ingrown toenails, nail discoloration, or thickened nails, all of which can become entry points for infection.
- Unusual odor: A foul smell from the feet can be an early sign of infection.
If you have difficulty seeing the bottoms of your feet due to limited flexibility, use a handheld mirror placed on the floor, or ask a family member to help with the inspection. There are even specially designed diabetic foot inspection mirrors available for this purpose.
Step 4: Moisturize — But Wisely
Diabetes often leads to dry skin on the feet, partly because the nerves that control oil and moisture production in the skin can be affected by neuropathy. Dry, cracked skin is more prone to developing fissures — deep cracks that can harbor bacteria and lead to infections.
- Apply a good-quality diabetic foot cream or lotion: Look for moisturizers containing urea, shea butter, glycerin, or lactic acid, which are especially effective at hydrating and softening diabetic skin.
- Apply to the top and bottom of the foot: Cover all surfaces of the foot except for the areas between the toes.
- Never moisturize between the toes: This is a crucial point. Applying lotion between the toes traps moisture and encourages fungal growth. Keep these areas dry.
- Moisturize immediately after washing and drying: Applying lotion to slightly damp skin helps lock in moisture more effectively.
- Avoid products with alcohol or fragrances: These can be overly drying and irritating to sensitive diabetic skin.
Step 5: Care for Your Toenails Properly
Toenail care is a surprisingly important component of diabetic foot health. Improperly trimmed nails can lead to ingrown toenails, cuts, and infections.
- Trim nails straight across: Cut your toenails straight across rather than in a curved shape. This prevents the edges from growing into the surrounding skin and causing ingrown toenails.
- Use a nail file to smooth edges: After trimming, use an emery board to file any sharp or rough edges to prevent them from cutting adjacent toes or snagging on socks.
- Don’t cut nails too short: Trimming nails too close to the skin increases the risk of cuts and ingrown nails.
- Trim in good lighting: Make sure you have adequate light when trimming nails to avoid accidental cuts.
- Never cut your own nails if you have poor circulation or neuropathy: If you have severely reduced sensation or circulation, toenail trimming should be done by a podiatrist to avoid accidental injury.
- Avoid cutting cuticles: Cuticles serve as a protective barrier against infection. Do not cut them.
Step 6: Choose and Wear the Right Footwear
The shoes and socks you wear every day play an enormous role in protecting your feet. Ill-fitting footwear is one of the leading causes of foot ulcers in diabetics, so this step deserves serious attention.
Choosing the Right Shoes
- Look for diabetic or therapeutic shoes: These are specially designed with extra depth, wider toe boxes, and cushioned insoles to reduce pressure points and accommodate foot deformities.
- Ensure a proper fit: Shoes should fit comfortably without pinching, rubbing, or leaving any part of the foot without support. Have your feet measured by a professional, as foot size can change over time.
- Choose shoes with a closed toe: Open-toed shoes, sandals, and flip-flops leave the feet vulnerable to injury. Diabetics should generally avoid these styles.
- Opt for soft, breathable materials: Leather and canvas uppers allow the foot to breathe and reduce moisture buildup.
- Break in new shoes gradually: Never wear new shoes for an extended period right away. Start with short periods and gradually increase the wearing time to identify any problem areas before they cause blisters.
- Always check inside shoes before putting them on: Use your hand to feel inside each shoe before wearing it. Seams, foreign objects, or folded insoles can cause significant damage to insensate feet.
Choosing the Right Socks
- Wear diabetic socks: These are specifically designed without tight elastic bands that can restrict circulation. They are typically seamless, padded, and made from moisture-wicking materials.
- Choose socks made from natural fibers: Cotton, wool, or bamboo socks help keep feet dry and comfortable.
- Avoid socks with seams over the toes: Seams can cause irritation and pressure sores in people with neuropathy who cannot feel the discomfort.
- Change socks daily: Fresh socks every day help keep the feet clean and reduce the risk of fungal infections.
- Never go barefoot: Even inside your home, always wear socks and shoes or protective footwear. A single step on a sharp object can lead to a serious wound that you may not feel.
Step 7: Manage Calluses and Dry Skin Safely
Calluses are areas of thickened skin that develop in response to repeated pressure or friction. While a small amount of callusing is normal, thick calluses can put excessive pressure on the skin beneath them, potentially leading to ulcers in diabetics.
- Use a pumice stone or emery board gently: After bathing when the skin is soft, gently rub areas of thickened skin with a pumice stone. Do not use it aggressively or to the point of pain.
- Never use sharp objects: Razor blades, scissors, or commercially available corn removers should never be used to trim calluses, as these can easily cause cuts and wounds.
- Never use chemical corn removers: Products containing salicylic acid are particularly dangerous for diabetics, as they can damage healthy skin surrounding a callus and cause chemical burns.
- See a podiatrist for significant calluses: If you have thick, persistent calluses, have them professionally managed by a podiatrist who specializes in diabetic foot care.
Step 8: Promote Healthy Circulation
Good blood flow to the feet is essential for healing and overall foot health. There are several things you can do throughout your day to encourage healthy circulation:
- Elevate your feet when sitting: Putting your feet up slightly when you’re seated helps blood flow back toward the heart. Avoid crossing your legs, which can restrict circulation.
- Wiggle your toes and rotate your ankles regularly: Simple exercises done several times throughout the day can help stimulate blood flow. Try ankle rotations, toe curls, and foot flexes.
- Walk regularly: Low-impact exercise like walking is one of the best ways to promote circulation in the legs and feet. Consult with your doctor about an appropriate exercise plan.
- Avoid smoking: Smoking severely constricts blood vessels and dramatically worsens peripheral circulation in diabetics.
- Avoid extreme cold: Cold temperatures cause blood vessels to constrict. Keep your feet warm with socks and appropriate footwear, but avoid using hot water bottles or heating pads, which can cause burns on insensate feet.
Weekly and Monthly Foot Care Habits
Beyond the daily routine, there are additional practices that should be incorporated on a weekly or monthly basis to maintain comprehensive foot health.
Weekly Habits
- Deep clean your footwear: Wipe out the insides of your shoes weekly to remove bacteria and moisture buildup. Allow them to air dry thoroughly.
- Rotate your shoes: Don’t wear the same pair of shoes every day. Rotating between two or more pairs allows each pair to fully dry between wearings and distributes pressure on the feet differently.
- Check the wear pattern on your shoes: Uneven wear can indicate gait problems or pressure points that may be contributing to callus formation or other foot issues.
Monthly Habits
- Assess your footwear: Check all of your shoes and socks for wear, damage, or changes in fit. Replace footwear that shows significant wear or no longer fits properly.
- Review your foot care products: Make sure your moisturizer, nail care tools, and other foot care products are clean, up to date,
Categories: