Introduction: Why Diabetic Foot Health Deserves Serious Attention
Living with diabetes means managing a complex web of health concerns, and among the most critical — yet often overlooked — is foot health. Diabetes can wreak havoc on the feet in ways that might seem minor at first but can escalate into severe, life-altering complications remarkably quickly. In fact, according to the American Diabetes Association, diabetic foot problems are one of the leading causes of non-traumatic lower limb amputations in the United States.
If you or a loved one has diabetes, knowing when to see a podiatrist for diabetic foot problems is not just helpful — it’s potentially life-saving. Podiatrists are medical specialists trained in the diagnosis, treatment, and prevention of foot and ankle conditions, making them an indispensable part of a comprehensive diabetes care team. This guide will walk you through everything you need to know about recognizing warning signs, understanding risk factors, and making the right call about when to seek specialized podiatric care.
Understanding How Diabetes Affects Your Feet
Before diving into the specific warning signs, it’s important to understand why diabetes puts your feet at such significant risk. Diabetes impacts foot health through two primary pathways:
Diabetic Peripheral Neuropathy
High blood sugar levels over time damage the nerves throughout the body, especially in the feet and legs. This condition, known as peripheral neuropathy, causes a loss of sensation that can make it impossible to feel pain, heat, or pressure. The danger here is profound: without the ability to feel pain, small injuries like blisters, cuts, or pressure sores can go completely unnoticed and deteriorate into serious wounds before you even realize something is wrong.
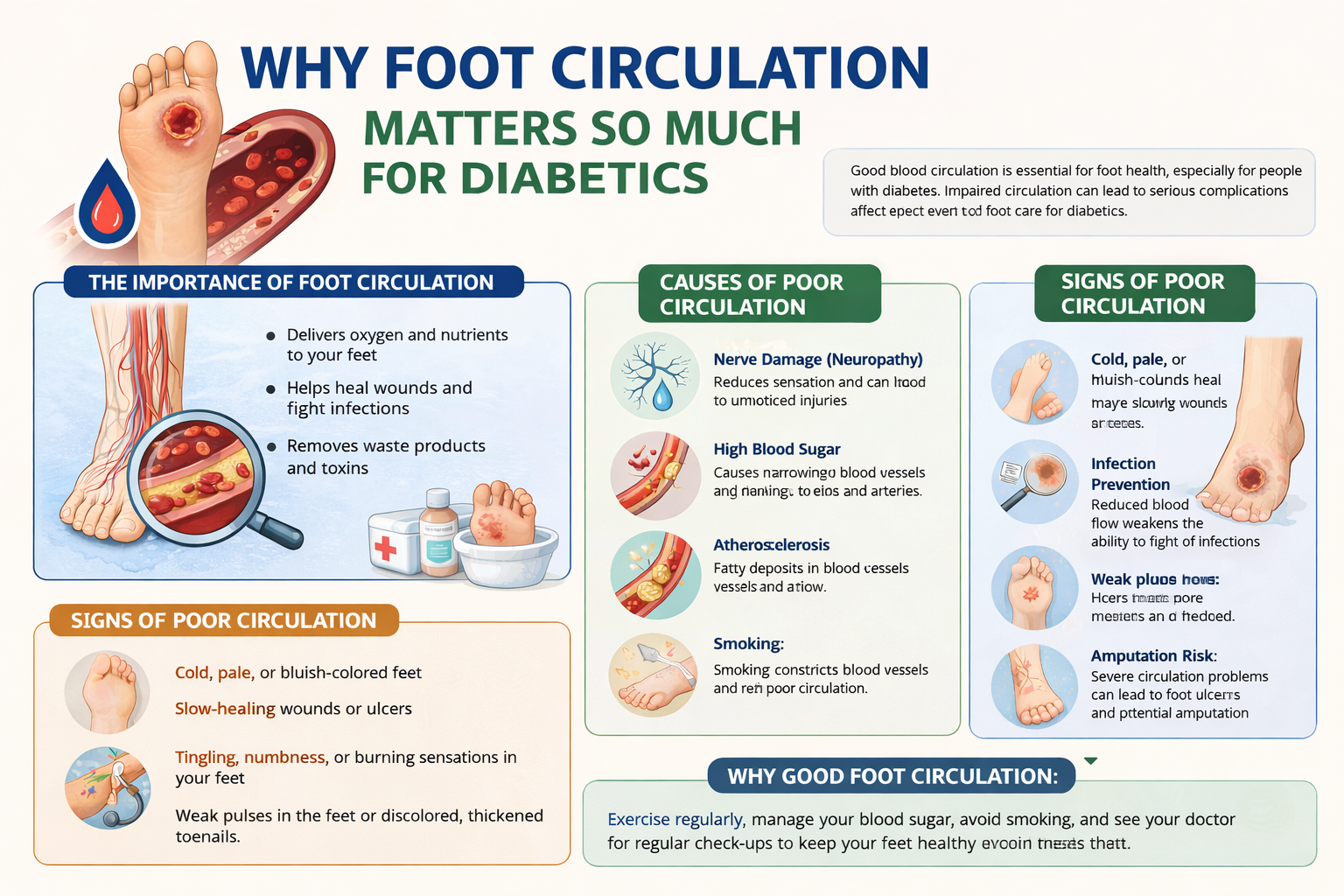
Peripheral Arterial Disease (PAD)
Diabetes also damages blood vessels, reducing circulation to the extremities. Poor blood flow means that even minor injuries heal slowly, if at all. Reduced circulation also makes the feet more vulnerable to infection, and it severely limits the body’s ability to fight off bacteria once an infection takes hold. The combination of neuropathy and poor circulation creates the perfect storm for dangerous diabetic foot complications.
Routine Podiatrist Visits: When Prevention Is the Best Medicine
One of the most important things to understand is that you don’t need to wait for a crisis to see a podiatrist. In fact, routine preventive care is the cornerstone of diabetic foot health. Most podiatrists and endocrinologists recommend that diabetics schedule regular foot checkups, even in the absence of symptoms.
How Often Should Diabetics See a Podiatrist?
The frequency of routine podiatrist visits depends on your individual risk level:
- Low risk (no neuropathy, good circulation, no foot deformities): At least once a year for a comprehensive foot exam.
- Moderate risk (some neuropathy or circulation issues): Every 3 to 6 months.
- High risk (history of ulcers, amputations, severe neuropathy, or PAD): Every 1 to 3 months, or as frequently as your podiatrist recommends.
During these routine visits, your podiatrist will check for signs of nerve damage, assess circulation, look for structural foot problems, trim nails, remove calluses, and provide personalized guidance on at-home foot care. These visits are a critical investment in your long-term health and can prevent minor problems from becoming major ones.
Warning Signs: When to See a Podiatrist Right Away
While routine visits are essential, there are also specific warning signs that should prompt you to call your podiatrist immediately — or in some cases, head to the emergency room. Never adopt a “wait and see” attitude when it comes to diabetic foot problems. What looks like a small issue today can become a limb-threatening emergency within days.
1. Any Open Wound, Cut, or Sore That Won’t Heal
Even a tiny cut or blister that fails to heal within a few days is a serious red flag for diabetic patients. Because of impaired circulation and neuropathy, wounds that would heal quickly in a healthy person can become chronic ulcers in someone with diabetes. Diabetic foot ulcers are the leading precursor to lower limb amputations, so any non-healing wound needs prompt professional evaluation.
Don’t attempt to treat open wounds at home with over-the-counter products and hope for the best. See your podiatrist as soon as possible for proper wound assessment and treatment.
2. Redness, Warmth, or Swelling in the Foot
These signs can indicate infection, inflammation, or even a serious condition called Charcot foot (discussed in more detail below). Redness and warmth that appear suddenly — especially if accompanied by swelling — should be evaluated by a podiatrist without delay. Do not assume it’s just a minor irritation or a sprain.
3. Signs of Infection
Infection in a diabetic foot can spread with alarming speed. Watch for the following signs of infection and seek immediate care if you notice any of them:
- Pus or discharge coming from a wound
- A foul or unusual odor from the foot
- Increasing redness or red streaks radiating from a wound
- Fever, chills, or feeling generally unwell alongside foot symptoms
- The wound deepening or worsening despite home care
In severe cases, a foot infection can progress to osteomyelitis (bone infection) or even sepsis, both of which are medical emergencies. If you notice signs of spreading infection along with systemic symptoms like fever, go to the emergency room immediately and follow up with your podiatrist.
4. Numbness, Tingling, or Burning Sensations
If you begin to notice new or worsening numbness, tingling, or a burning sensation in your feet, this may indicate the onset or progression of peripheral neuropathy. These symptoms are often described as a “pins and needles” feeling or a sensation like wearing socks when you’re not. While these symptoms may seem minor, they signal that your protective sensation is diminishing — meaning you’ll be less able to detect future injuries. A podiatrist can assess the severity of neuropathy and implement protective measures to minimize your risk.
5. Foot Pain at Rest or at Night
Pain that occurs when you’re resting, particularly at night, can be a sign of severe peripheral arterial disease. This is known as “rest pain” and indicates significantly reduced blood flow to the feet. This is a serious vascular concern that needs prompt evaluation. Your podiatrist may work in conjunction with a vascular specialist to address circulation problems.
6. Changes in Skin Color
Unusual changes in the color of your foot or toes are important warning signs that should never be ignored. Specifically, look out for:
- Pale or white skin: May indicate reduced blood flow
- Blue or purple discoloration: Can signal poor oxygenation or circulatory compromise
- Dark or black skin: May indicate gangrene, a life-threatening emergency requiring immediate medical care
- Persistent redness: Could indicate infection or Charcot foot
Any unexpected or progressive color change in the feet warrants same-day contact with your podiatrist or a visit to the emergency room if gangrene is suspected.
7. Thickened or Ingrown Toenails
For people without diabetes, an ingrown toenail might be a painful nuisance that resolves on its own or with simple home care. For someone with diabetes, however, an ingrown toenail can quickly become infected and lead to serious complications. Similarly, thickened toenails — which are common in diabetics — can increase pressure on the nail bed and lead to injury. Never attempt to cut or treat ingrown or thickened toenails yourself if you have diabetes. Always have a podiatrist handle nail care to ensure it’s done safely.
8. Calluses or Corns That Are Thickening or Bleeding
Calluses are common in diabetics and often develop due to uneven pressure distribution on the feet. While a thin callus might not be immediately dangerous, thick calluses can hide ulcers forming underneath them, or they can crack and become entry points for bacteria. Bleeding calluses or corns are especially concerning. A podiatrist can safely debride (remove) callus tissue and assess whether there is any underlying damage.
9. Foot Deformities or Changes in Foot Shape
Conditions like hammertoe, bunions, claw toe, or a more serious deformity known as Charcot foot can dramatically alter the biomechanics of walking, creating new pressure points that lead to ulcers. If you notice your foot is changing shape, developing new prominences, or if your shoes no longer fit properly, see a podiatrist. They can recommend custom orthotics, appropriate footwear, and — in some cases — surgical intervention to prevent further complications.
10. A Blister or Pressure Sore
Something as seemingly trivial as a blister from new shoes can become dangerous in the context of diabetes. Because of neuropathy, you might not even feel the blister forming. If you discover a blister — especially one that has broken open — on your foot, clean it gently and contact your podiatrist for guidance. Do not attempt to pop intact blisters, as this introduces the risk of infection.
Charcot Foot: A Diabetic Emergency You Must Know About
Charcot foot (also called Charcot arthropathy) is a severe and often underrecognized complication of diabetic neuropathy that deserves special mention. In this condition, the bones of the foot weaken to the point where they fracture and dislocate, sometimes with surprisingly little pain due to neuropathy. The affected foot typically becomes red, swollen, and warm — symptoms that can be mistaken for an infection or sprain.
Without prompt treatment, Charcot foot can cause the foot to collapse into a “rocker-bottom” deformity, which creates severe pressure points and dramatically increases the risk of ulceration and amputation. If you have diabetes and your foot suddenly becomes red, swollen, and warm — even without significant pain — treat it as an emergency and see a podiatrist immediately. Early diagnosis and offloading (often with a cast or specialized boot) can prevent permanent deformity.
After an Amputation: Ongoing Podiatric Care Is Essential
For those who have already experienced a diabetic foot amputation — whether of a toe, part of the foot, or a limb — ongoing podiatric care becomes even more critical. An amputation changes the mechanics of how you walk and increases pressure on remaining foot structures, elevating the risk of new ulcers and further complications. Your podiatrist will play a vital role in:
- Monitoring the residual limb for complications
- Fitting appropriate prosthetics or orthotics
- Preventing ulcers on the remaining foot
- Providing rehabilitation guidance
People who have had one amputation are at significantly higher risk for another, making regular podiatric follow-up non-negotiable.
What Happens During a Diabetic Foot Exam?
If you’ve never seen a podiatrist for diabetic foot care, you might wonder what to expect. A comprehensive diabetic foot examination is thorough and covers multiple aspects of foot health:
- Neurological assessment: Testing sensation with a monofilament, tuning fork, or pin to detect neuropathy
- Vascular assessment: Checking pulses in the foot and ankle, potentially using Doppler ultrasound to assess blood flow
- Skin assessment: Examining for dryness, cracks, calluses, corns, ulcers, or infection
- Nail assessment: Checking for ingrown nails, fungal infections, or thickening
- Structural assessment: Evaluating foot shape, joint mobility, and identifying any deformities
- Footwear evaluation: Reviewing your shoes for proper fit and support
- Education: Discussing proper at-home foot care, nail trimming technique, appropriate footwear, and when to seek urgent care
Finding the Right Podiatrist for Diabetic Foot Care
Not all podiatrists have the same level of experience with diabetic foot care, so it’s worth seeking out a provider who specializes in or has extensive experience with diabetic patients. Here are some tips for finding the right podiatrist:
- Ask your primary care physician or endocrinologist for a referral
- Look for a podiatrist who is a member of the American Podiatric Medical Association (APMA)
- Check if the podiatrist has experience with wound care, orthotics, and diabetic foot management
- Confirm that the podiatrist accepts your insurance plan
- Consider whether the podiatrist is affiliated with a hospital or wound care center for comprehensive care access
Ideally, your podiatrist should work collaboratively with your primary care doctor, endocrinologist, vascular surgeon, and other members of your healthcare team to provide integrated, holistic diabetic care.
At-Home Foot Care: What You Should Be Doing Between Visits
While professional podiatric care is irreplaceable, daily at-home foot care plays a major role in preventing complications. Your podiatrist will likely provide personalized recommendations, but general best practices include:
- Inspect your feet daily: Use a mirror to check the bottoms of your feet, or ask a family member to help. Look for cuts, blisters, redness, swelling, or any changes.
- Wash and dry your feet carefully: Use lukewarm (not hot) water and mild soap. Dry thoroughly, especially between the toes, where moisture can promote fungal infections.
- Moisturize the skin: Apply lotion to the tops and bottoms of your feet to prevent cracking, but avoid applying between the toes.
- Wear appropriate footwear: Always wear well-fitting, cushioned shoes and clean, dry socks. Never walk barefoot, even indoors.
- Manage blood sugar levels: Keeping blood glucose under control is the single most effective way to prevent neuropathy and circulatory complications from worsening.
- Don’t use heating pads or hot water bottles on your feet: Neuropathy makes it difficult to gauge temperature, increasing burn risk.
- Quit smoking: Smoking significantly worsens peripheral arterial disease, further reducing blood flow to the feet.
The Cost of Waiting: Why Early Intervention Matters
Many people delay seeing a podiatrist because they feel their symptoms are too minor to warrant a visit, they’re concerned about the cost, or they simply don’t realize how serious their situation is. Unfortunately, this delay can come at an enormous price. Studies consistently show that early intervention dramatically reduces the rate of diabetic amputations. Treating a small ulcer in its early stages is far less costly — financially and physically — than treating an advanced infection, undergoing surgery, or managing life after amputation.
Medicare and most insurance plans cover podiatric care for diabetic patients, particularly for routine foot exams and nail care when neuropathy is documented. Check with your insurance provider to understand your coverage, and don’t let cost concerns stop you from seeking the care you need.